How much does Medicare pay for physical therapy
This article will specifically reference the Medicare Part B Physician Fee Schedule look-up tool to determine how much does Medicare pay for physical therapy.
Medicare Part B payment rates for a physical therapy initial evaluation CPT code 97161?
Medicare Part B has reduced physical therapy rates from $98.01 in 2021 to $95.13 in 2023. This change is specifically for outpatient physical therapy reimbursement in the state of Ohio.
To determine Medicare Part B reimbursement allowed amounts for the calendar year and geographic location you will need to either go to your local MAC website and search their physician fee schedule, or you can find the same information on the CMS website under Physician Fee Schedule Look-Up Tool.
Below is a table showing Medicare Part B allowed amounts for participating providers in Ohio.
Medicare allowed amount by CPT Code: 97110, 97530, and 97140?
Below is a table containing the CMS Physician Fee Schedule allowed amounts for participating physical therapy providers. This table compares reimbursement rates between 2023 and 2021 for Ohio’s CGS Medicare.
Reimbursement will vary by state so it is important that you choose your specific MAC or location.
You can see that the Medicare Part B participating provider allowed amounts are as follows:
| CPT Code | 2023 Payment | 2021 Payment |
| 97110 | $27.89 | $29.21 |
| 97112 | $31.96 | $33.82 |
| 97140 | $25.72 | $26.92 |
| 97161 | $95.13 | $98.01 |
| 97530 | $34.80 | $37.46 |
What is the difference between Facility and Non-Facility Price?
Physical therapists, occupational therapists, and speech-language pathologists in private practice use the Non-facility price to estimate the allowed amount.
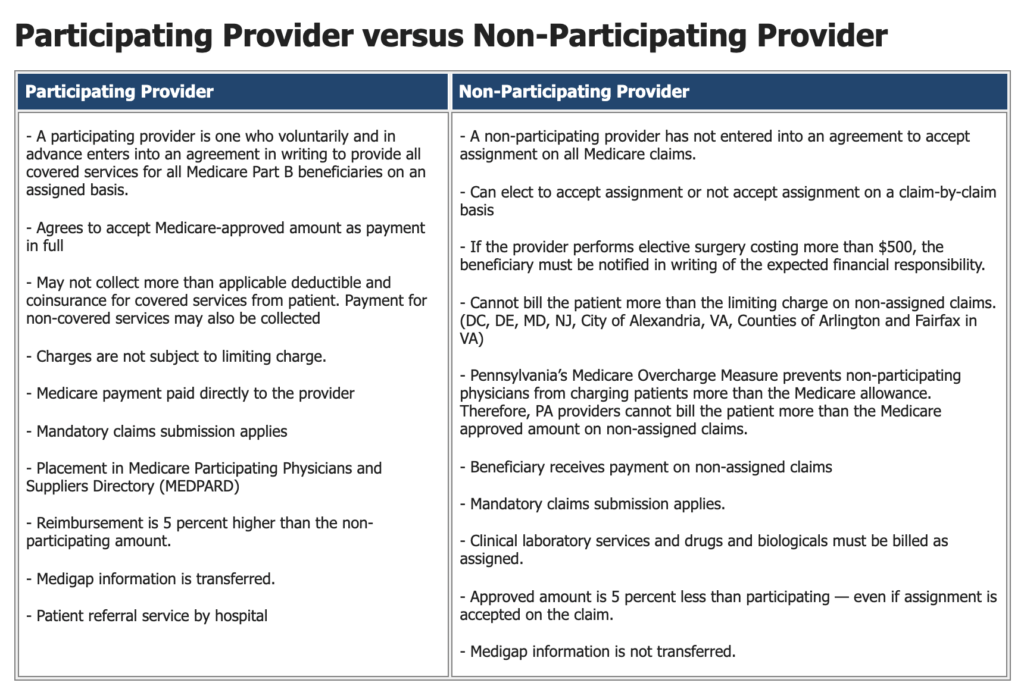
What is the difference between PAR and NonPAR allowed amounts?
The NonPAR allowed amount is 95% of the PAR allowed amount.
* Source: Novitas-Solutions
Is it better for a physical therapist to be PAR or NonPAR?
In my opinion, it is NOT better for a physical therapist, occupational therapist, or speech-language pathologist to be Non-PAR (non-participating).
In the following video, I will share the reasons why Non-PAR is not better, but to summarize it here I have created a list:
- Both participating and non-participating providers are required to comply with all of the same Medicare regulations.
- Both participating and non-participating providers are required to submit claims on behalf of the beneficiary for covered services, but Non-PAR claims are not automatically forwarded to the patient’s supplemental insurance.
- Yes, it is true the Non-PAR provider may choose not to accept assignment and charge the Medicare beneficiary up to 115% of the Non-PAR fee schedule, but the Non-PAR fee schedule is lower and the provider must collect from the patient either at the time of service or after. This results in increased administrative costs.
- If a single Medicare beneficiary chooses not to pay a Non-PAR provider then the cost of collections and other measures may eliminate the potential small increase in reimbursement.
Does Medicare Part B have a CAP on Physical Therapy Services?
No, Medicare Part B no longer has a cap. Now it is referred to as a financial threshold. Click here for information directly from CMS.
In 2023 the Medicare financial threshold for occupational therapy services is $2,230.
The Medicare financial threshold for physical therapy and speech-language pathology combined is $2,230.
What happens if physical therapy services exceed the financial threshold?
If therapy services continue to be medically necessary based on established CMS guidelines, local MAC published guidelines, and the clinical judgement of the provider, then the KX modifier may be added to the CPT code claim line item and payment will be issued from Medicare.
If therapy services are deemed no longer medically necessary AND the patient wants to continue to receive therapy services while paying out of pocket then the provider may choose to issue a mandatory advanced beneficiary notice (ABN) before continuing care.
What if a Medicare beneficiary does not have a secondary insurance plan?
If the Medicare beneficiary does not have a secondary insurance policy that Medicare part B will cover 80% of the allowed amount and the patient will be responsible to pay the remaining 20%.
The best practice for the physical therapist in this situation is to estimate the 20% coinsurance and collect that amount from the patient at the time of service.
After Medicare has processed the claims the physical therapist may review the Medicare determined 20% patient responsibility and either refund the patient if more than expected was collected or invoice the patient if a remaining balance exists.
Does a Medicare secondary insurance plan pay for out-of-network physical therapy?
A traditional Medicare supplemental plan in the secondary position will pay therapists contracted with Medicare just the same as if the therapist was contracted with the supplemental payer.
But non-supplemental secondary insurance plans are not required to pay non-contracted therapists. Each plan is different so you will need to verify coverage and determine any patient responsibility before delivering treatment.
How can I learn more?
The first Tuesday of each month I start a new LIVE cohort of students in my Zero to Paid Medicare Billing Course. For more information on the course visit this website’s homepage.
Additional and Related Article Links:
- How to apply for a Type 2 NPI
- How to INCREASE the Average Physical Therapist Salary
- 5 Best Books For Starting A New Physical Therapy Practice in 2021

Anthony Maritato, PT
Physical Therapist / Private Practice Owner
As a serial entrepreneur since the age of 7, Anthony (Tony) Maritato didn’t start his first physical therapy clinic until he was 26.
After recently graduating from Pennsylvania State University with a bachelor’s degree in Kinesiology, Tony fell in love with the profession of physical therapy. Not wanting to wait until getting his degree in Physical Therapy, Tony quickly opened a personal training studio which transitioned to a full-time physical therapy clinic once he recruited his now-wife, Kathy Long Maritato, PT.
Since then Kathy and Tony have grown Total Therapy Solutions LLC into a successful private practice with two locations in Ohio.
Tony spends his free time teaching other therapists how to contract with and bill Medicare for outpatient therapy services.
25 Most Commonly Used Physical Therapy Abbreviations
25 Most Common Outpatient Physical Therapy Abbreviations in 2022 AAROM - Active Assisted Range of Motion AROM - Active Range of Motion CLOF - Current Level of Function CPM - Continuous Passive Motion DPT - Doctor of Physical Therapy ER - External Rotation GLOF - Goal...

PT vs PTA: Should I become a PT or PTA?
Should I Become a PT vs PTA in 2023? This is a great question. In my opinion, the main difference between choosing to become a PT vs PTA depends on your goals for the future. There is little difference in the salary, job opportunities, and fulfillment of both paths....
Will PTAs Be Phased Out in 2023?
Will PTAs be phased out of the physical therapy profession in 2023? Absolutely not! Physical therapist assistants are a vital part of the patient care experience. I believe the best way to preserve the future of physical therapist assistants in the physical therapy...

Can you Charge a Medicare Patient for a No Show Fee? 2022 Update
Can You Charge a No Show Fee to a Medicare Beneficiary? Yes, you are allowed to charge a no show fee to a Medicare beneficiary as long as you have an established no show fee policy for all patients at your practice. "According to Chapter 1, section 30.3.13 of the...

CPT Code 95992
CPT Code 95992 CPT 95992 – Canalith repositioning procedure(s) (eg, Epley maneuver, Semont maneuver), per day* Source: NGS A56566 Appropriate Diagnosis to Charge CPT Code 95992 H81.11 - Benign paroxysmal vertigo, right ear H81.12 - Benign paroxysmal vertigo, left ear...

Reason Code 4 | Remark Code N519 Physical Therapy Denial
Reason Code 4 Medicare Remarks: "The procedure code is inconsistent with the modifier used or a required modifier is missing." The most common reason for this denial is a missing professional discipline modifier. GP Modifier Physical Therapy GO Modifier Occupational...

How to Confirm a PT Patient has Traditional Medicare vs Medicare Advantage
Traditional Medicare vs Medicare Advantage Plans Medicare Part B Traditional Medicare is often referred to as Medicare Part B. This plan pays for outpatient services which include physical therapy in private practice. Medicare Part C Medicare Advantage plans are...

Medicare ABN Form: Physical Therapist In Private Practice
What is a Medicare ABN Form? According to the Medicare Claims Processing Manual Chapter 30 Section 50: " The ABN is an Office of Management and Budget (OMB)-approved written notice issued by healthcare providers and suppliers for items and services provided under...

Physical Therapy Medical Record Retention Laws in 2022
Medical Record Retention Law Question: "Can someone point me to the resources for how long to maintain medical records? "Currently, in 2022, the longest duration you must store medical records is 10 years according to § 3731. False claims procedure.How long is a...

Physical Therapist Vacation Coverage | CMS Locum Tenens Guidelines 2022
Physical Therapist Vacation Coverage Options? There are 2 primary options that exist for a private practice physical therapy clinic to hire an outside physical therapist to treat Medicare beneficiaries while another physical therapist is on vacation, maternity leave,...